What is Pelvic Instability?
Pregnancy is a beautiful and transformative journey, but it can also bring about various physical challenges. As the body adapts to accommodate a growing baby, many people experience discomfort and pain in the pelvic region. Pelvic instability encompasses a broad range of conditions that cause pain and discomfort in the pelvic region during pregnancy. It can involve a combination of SI joint dysfunction, Symphysis Pubic Diastasis (SPD), and generalized ligamentous laxity. Pelvic instability often leads to difficulties with mobility and impacts daily activities. Pelvic instability is usually caused by hormonal changes which increase ligamentous laxity in the pelvis. The laxity accompanied by the growing baby’s weight can contribute to pain in the pubic region, difficulty walking, and discomfort during certain movements. The ligamentous laxity in the pelvis is helpful during labor and delivery, but can cause a lot of discomfort in the preceding months.
Pelvic instability during pregnancy can lead to additional complications, such as sciatica and nerve irritation. The pelvic region houses a network of nerves, including the sciatic nerve, which extends from the lower back down the legs. When the pelvis becomes unstable, it can put pressure on the nerves, leading to symptoms such as shooting pain, tingling, or numbness along the sciatic nerve pathway. This condition is commonly referred to as sciatica.
It is crucial to seek professional guidance from a physical therapist or healthcare provider if you experience symptoms of sciatica or nerve irritation during pregnancy. They can assess your condition, provide appropriate interventions, and guide you through exercises and stretches that will help alleviate nerve-related discomfort.
Remember, everyone’s experience during pregnancy is unique, and the severity of symptoms may vary. The key is to address pelvic instability and associated nerve issues promptly and with the guidance of healthcare professionals to ensure a comfortable and healthy pregnancy journey.
Symphysis Pubic Diastasis (SPD)
Symphysis Pubic Diastasis (SPD) is a condition characterized by the separation or widening of the pubic symphysis, the joint located at the front of the pelvis where the pubic bones meet. Sometimes this condition is called, “lightening crotch” because it can cause sharp groin pain with positional changes. During pregnancy, hormonal changes, particularly the hormone relaxin, cause the ligaments in the pelvic region to loosen. This is a natural process that allows the pelvis to accommodate the growing baby and facilitates childbirth. However, in some cases, the pubic symphysis can become excessively lax, leading to SPD.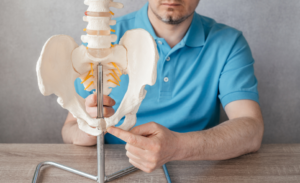
Symptoms of SPD: Women with SPD may experience a range of symptoms, including:
- Pubic pain: Pain in the pubic area is the primary symptom of SPD. It can vary from mild discomfort to severe pain that radiates to the groin, lower abdomen, hips, or lower back. The pain may worsen with activities such as walking, rolling over in bed, climbing stairs, or spreading the legs.
- Difficulty with weight-bearing activities: Women with SPD may find it challenging to perform weight-bearing activities like standing, walking, or getting in and out of a car due to the instability and pain in the pelvis.
- Clicking or popping sensation: Some women may experience a clicking or popping sensation in the pubic area during certain movements or transitions.
- Difficulty with certain positions: Activities such as getting in and out of a car or getting up from a chair may be uncomfortable or painful.
Management and Physical Therapy Interventions for SPD
Physical therapy plays a crucial role in managing SPD during pregnancy. A physical therapist specializing in pelvic health can provide tailored interventions based on the individual’s specific needs. Here are some common strategies used in physical therapy for SPD:
- Manual therapy: Therapists may use gentle manual techniques to help realign and stabilize the pubic symphysis. These techniques can include gentle mobilizations, soft tissue massage, and myofascial release to reduce pain and improve joint function.
- Pelvic floor muscle exercises: Strengthening the pelvic floor muscles can provide additional stability to the pelvis. Physical therapists provide guidance in performing appropriate exercises that engage the pelvic floor muscles, such as Kegels.
- Stabilization exercises: Targeted exercises are prescribed to strengthen the muscles surrounding the pelvis, including the hip abductors, glutes, and core muscles. These exercises help improve overall pelvic stability and reduce strain on the pubic symphysis.
- Pain management techniques: Therapists may utilize various pain management modalities, such as heat or cold therapy, or TENS (Transcutaneous Electrical Nerve Stimulation), to alleviate discomfort and promote healing.
- Education and activity modification: Physical therapists educate women about proper body mechanics, postural alignment, and strategies to modify daily activities to minimize stress on the pubic symphysis. They may recommend techniques such as using a pillow between the legs while sleeping, avoiding activities that exacerbate symptoms, and providing guidance on safe movement patterns during pregnancy.
- Stability belt recommendations: Stability belts, also known as maternity support belts or belly bands or Serola Belts, are external devices designed to provide additional support to the abdominal and pelvic region during pregnancy. These belts can help alleviate pressure on the SI joints, reduce pubic symphysis separation, and provide support to the growing belly.

It is important to note that the severity of SPD can vary among individuals, and treatment plans should be tailored accordingly. In some cases, the use of assistive devices, such as crutches or a pelvic support belt, may be recommended to reduce stress on the pubic symphysis and provide additional support.